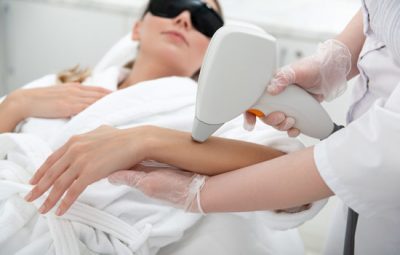
 Our healthcare and business law firm works with healthcare providers and businesses to open cosmetic medical and wellness spas. The medical spa entity has grown drastically over the past few years. Some states and medical boards have developed laws and rules governing medical and wellness spas. As medical and wellness spas continue to grow, we can anticipate more laws and rules governing medical and wellness spas. On July 19, 2023, the Alabama Board of Medical Examiners (“Medical Board”) published changes to the rules governing the “Use of Lasers and Other Modalities,” which can be found in Chapter 540-X-11 of the Rules of the Medical Board. The rule is broken down into many different categories. This post provides an overview of the rule changes that are potentially applicable to medical spa practitioners. If you have a question about the Alabama Medical Board’s rules or would like to discuss this blog post, you may contact our healthcare and business law firm at (404) 685-1662 (Atlanta) or (706) 722-7886 (Augusta), or by email, info@hamillittle.com. You may also learn more about our law firm by visiting www.hamillittle.com.
Our healthcare and business law firm works with healthcare providers and businesses to open cosmetic medical and wellness spas. The medical spa entity has grown drastically over the past few years. Some states and medical boards have developed laws and rules governing medical and wellness spas. As medical and wellness spas continue to grow, we can anticipate more laws and rules governing medical and wellness spas. On July 19, 2023, the Alabama Board of Medical Examiners (“Medical Board”) published changes to the rules governing the “Use of Lasers and Other Modalities,” which can be found in Chapter 540-X-11 of the Rules of the Medical Board. The rule is broken down into many different categories. This post provides an overview of the rule changes that are potentially applicable to medical spa practitioners. If you have a question about the Alabama Medical Board’s rules or would like to discuss this blog post, you may contact our healthcare and business law firm at (404) 685-1662 (Atlanta) or (706) 722-7886 (Augusta), or by email, info@hamillittle.com. You may also learn more about our law firm by visiting www.hamillittle.com.
Rule 540-X-11 “Guidelines for the Use of Lasers and Other Modalities Affecting Living Tissue” has been a rule in Alabama since 2007. However, on March 16, 2023, the Medical Board passed changes and additions to the Rule, which became effective on July 17, 2023. The deadline for compliance with the provisions is July 17, 2024.
Although the Medical Board made many changes, an important change to the rules is that these rules apply to many cosmetic lasers including cryotherapy, infrared lasers, radiofrequency micro-needling, Class III lasers that work on heat-based targeting of skin and collagen. The Medical Board made many changes to Rule 540-X-11. The Medical Board made many notable changes to the rule that may apply to med spa practitioners, including as follows:
 Total Health Law Blog
Total Health Law Blog


 Our healthcare and business law firm works with healthcare providers and businesses to
Our healthcare and business law firm works with healthcare providers and businesses to  Our healthcare and business law firm consistently works with physicians who are dealing with complications resulting from adverse reporting to the National Practitioner Data Bank (“NPDB”). A previous blog post outlines the process for disputing an NPDB report. Although difficult, our law firm has had success in appeals to HHS resulting in void reports. This post provides more information about the process of disputing a report directly with HHS and what occurs with a successful resolution. If you have a question about the NPDB or would like to discuss this blog post, you may contact our healthcare and business law firm at (404) 685-1662 (Atlanta) or (706) 722-7886 (Augusta), or by email,
Our healthcare and business law firm consistently works with physicians who are dealing with complications resulting from adverse reporting to the National Practitioner Data Bank (“NPDB”). A previous blog post outlines the process for disputing an NPDB report. Although difficult, our law firm has had success in appeals to HHS resulting in void reports. This post provides more information about the process of disputing a report directly with HHS and what occurs with a successful resolution. If you have a question about the NPDB or would like to discuss this blog post, you may contact our healthcare and business law firm at (404) 685-1662 (Atlanta) or (706) 722-7886 (Augusta), or by email,  Our healthcare and business law firm consistently works with physicians who are dealing with complications resulting from adverse reporting to the National Practitioner Data Bank (“NPDB”) as well as entities in deciding what reports may be appropriate for certain situations. Whether you are on the side of the provider or reporting entity, it is important to understand the types of NPDB reports that are permitted. This post outlines the four types of reports. If you have a question about the NPDB or would like to discuss this blog post, you may contact our healthcare and business law firm at (404) 685-1662 (Atlanta) or (706) 722-7886 (Augusta), or by email,
Our healthcare and business law firm consistently works with physicians who are dealing with complications resulting from adverse reporting to the National Practitioner Data Bank (“NPDB”) as well as entities in deciding what reports may be appropriate for certain situations. Whether you are on the side of the provider or reporting entity, it is important to understand the types of NPDB reports that are permitted. This post outlines the four types of reports. If you have a question about the NPDB or would like to discuss this blog post, you may contact our healthcare and business law firm at (404) 685-1662 (Atlanta) or (706) 722-7886 (Augusta), or by email,  Our healthcare and business law firm consistently works with physicians who are dealing with complications resulting from adverse reporting to the National Practitioner Data Bank (“NPDB”). Certain entities, including medical licensure boards, facilities with a peer review process, and medical malpractice payers, have a duty to
Our healthcare and business law firm consistently works with physicians who are dealing with complications resulting from adverse reporting to the National Practitioner Data Bank (“NPDB”). Certain entities, including medical licensure boards, facilities with a peer review process, and medical malpractice payers, have a duty to  Our healthcare and business law firm works with healthcare providers and businesses to
Our healthcare and business law firm works with healthcare providers and businesses to  Our healthcare and business law firm works with many providers and other allied health professionals who are beginning their journeys of opening a Medical Spa. Medical Spas have been
Our healthcare and business law firm works with many providers and other allied health professionals who are beginning their journeys of opening a Medical Spa. Medical Spas have been  At the beginning of COVID-19, telemedicine rules were softened on the state and federal level. In a
At the beginning of COVID-19, telemedicine rules were softened on the state and federal level. In a 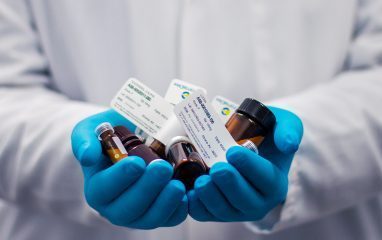 As a healthcare and business law firm, many of our clients come to us with questions relating to the proper ordering and management of controlled substances. As such, we wanted to take this opportunity to point out a recent update to the DEA’s Practitioner’s Manual.
As a healthcare and business law firm, many of our clients come to us with questions relating to the proper ordering and management of controlled substances. As such, we wanted to take this opportunity to point out a recent update to the DEA’s Practitioner’s Manual.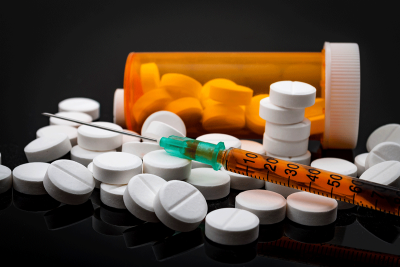 Our healthcare and business law firm works with many physicians in Georgia who are facing mental health and substance abuse difficulties. Sometimes those difficulties bleed into work and can cause work and/or licensure issues. Georgia offers an incredible resource dedicated to physician recovery in a way that protects Georgia citizens and minimizes career concerns for the physician—the Georgia Professional Health Program (“PHP”). This post provides 3 Facts about the Georgia PHP. If you are experiencing or are concerned about ramifications of a potential addiction or mental health disorder, in addition to seeking medical help, we recommend contacting an experienced attorney who can assist you through this difficult process and help minimize potential licensure and career impacts. If you have questions regarding this blog post or would like to speak with counsel regarding
Our healthcare and business law firm works with many physicians in Georgia who are facing mental health and substance abuse difficulties. Sometimes those difficulties bleed into work and can cause work and/or licensure issues. Georgia offers an incredible resource dedicated to physician recovery in a way that protects Georgia citizens and minimizes career concerns for the physician—the Georgia Professional Health Program (“PHP”). This post provides 3 Facts about the Georgia PHP. If you are experiencing or are concerned about ramifications of a potential addiction or mental health disorder, in addition to seeking medical help, we recommend contacting an experienced attorney who can assist you through this difficult process and help minimize potential licensure and career impacts. If you have questions regarding this blog post or would like to speak with counsel regarding